For professionals
Шановні колеги, дорогі друзі!
Хочеться сподіватися, що агресивна війна, започаткована Росією, скоро закінчиться на політичних умовах України.
Але навіть тоді, коли закінчиться війна, роботи нам, ортопедам, вистачить на довгі роки.
Адже основні пошкодження, з якими ми маємо справу, це навіть не вогнепальні, а мінно-вибухові поранення. З великими дефектами як м’яких тканин, так і кістки. Заміщення дефектів, м’якотканинна та кісткова пластика, боротьба з інфекцією – це основні напрямки нашої роботи.
Уряд та шпиталі в Україні намагаються купувати нам багато необхідного, але в бюджеті часто не вистачає коштів.
І ми вдячні всім вам, дорогі друзі, за допомогу. Саме завдяки гуманітарній підтримці ми маємо можливість використовувати сучасні зовнішні та внутрішні фіксатори, користуватися якісним інструментом, використовувати системи RIA та сучасні замінники кістки з антибактеріальним ефектом (типу BonaLive).
Дякуючи Вам на цій сторінці ми будемо публікувати випадки порятунку кінцівок, що стало можливими в тому числі завдяки вашій допомозі.
А до колег прохання, – користуватися випадками можна із зазначенням авторства. Дякую за підтримку!
Петро Нікітін
Начальник відділення травматології головного клінічного шпиталю прикордонної служби України.
Почесний член правління АО Травма Украïна
Андрій Волна
травматолог-ортопед, волонтер,
Почесний член Ради піклувальників АО Фонду
Dear colleagues, dear friends!
We would like to hope that the aggressive war launched by Russia will soon end on the political terms of Ukraine.
But even when the war ends, we, orthopedic surgeons, will have enough work for many years.
After all, the main injuries we deal with are not even gunshot fractures, but blast injuries. With large bone and soft tissues defects.
Bone defects treatment, soft tissue plastic surgery, and the fight against infection are the main field of our deal today.
The government and hospitals in Ukraine are trying to buy a lot of what we need, but the budget often lacks funds during the war.
And we are grateful to all of you, dear friends, for your help. It is thanks to humanitarian support that we have, we could use modern external and internal fixators, use high-quality instruments, use RIA systems and modern bone substitutes with an antibacterial effect (such as BonaLive).
Thanking you on this page we will publish cases of limb saving, which became possible to treat thanks to your help.
Dear colleagues, if you would like to use these cases for educational needs, please don’t forget the indication of authorship.
Thank you for your support!
Petro Nikitin
Chief of Traumasurgical Department of the Main Military Clinical Hospital of the Border Guard Service of Ukraine
Honorary Member of the Board of AO Trauma Ukraine
Andrey Volna
Trauma and orthopedic surgeon, volunteer
Senior Trustee of AO Foundation

16.07.2025 Case 2
TO SAVE OR TO AMPUTATE?
(Mangled extremity management during the war)
This is not as simple a question as it may seem at first glance.
Of course — save it! you might say.
But let’s take a closer look.
What does limb salvage mean in the context of severe blast injury?
Typically, it involves a series of consecutive surgical procedures interspersed with stages of rehabilitation.
Sometimes this concept is difficult for healthcare bureaucrats (in any country) to understand. For them, everything should be straightforward: first aid, life-saving interventions, fracture stabilization (or amputation) and stage of rehabilitation then.
However, multi-stage surgeries to salvage a severely injured limb — alternating with rehabilitation phases and sometimes long pauses (several weeks or even months for antibiotic therapy) — don’t always fit into that linear logic.
Are there studies on this topic? Absolutely.
I’ve had the opportunity to give lectures on this issue — in Ukraine, Turkey, and elsewhere (I don’t recall exactly where).
So, without going into too much technical detail for a general audience, I’ll say that perhaps the most respected and frequently cited study on this topic is the Lower Extremity Assessment Project (LEAP).
This was a prospective, comprehensive study (NIH-funded — about $6 million) that examined high-energy lower limb injuries that were threatening to result in amputation. It included 601 patients across 8 Level I trauma centres.
Of course, no study can offer a definitive recommendation — save or amputate — as the number of influencing factors (medical, social, organizational, etc.) is simply too great.
But here are some key takeaways that might be useful for reflection:
- Neither amputation nor prolonged treatment of a mangled limb leads to full recovery.
- In cases of lower limb amputation, 53% of patients returned to work, compared to 47% after reconstruction.
- 48% of patients undergoing reconstruction required repeat hospitalizations — which is expected. But even among amputees, 34% required re-hospitalization. In other words, while amputation solves some problems, it also creates new ones.
(Bosse MJ, MacKenzie EJ, Kellam JF, et al. An analysis of outcomes of reconstruction or amputation after leg-threatening injuries. N Engl J Med. 2002 Dec 12;347(24):1924–1931.)
But here’s what’s crucial:
While amputation may seem like a simpler, cheaper, and “quicker” solution early in the treatment of a severely injured patient, over time, the life of an amputee becomes more and more expensive. This includes medical, social, and direct financial burdens on the family.
Consider this:
Over the lifetime of a patient (in developed countries with high levels of social support), the total cost of surgical treatment, medical care, and maintaining a normal life for a person with a salvaged limb is about $163,000 USD.
For someone with an amputated lower limb, it’s about $509,000 USD.
(MacKenzie EJ, Jones AS, Bosse MJ, et al. Health-care costs associated with amputation or reconstruction of a limb-threatening injury. J Bone Joint Surg Am. 2007 Aug;89(8):1685–1692.)
That’s an enormous difference.
This is why limb salvage, especially in young patients and particularly when one of the lower limbs has been irreversibly lost (this is quite typical when anti-personnel mines explode), is a top priority for us.
You can help support the limb salvage efforts for wounded Ukrainian soldiers by donating via the following details (also available in the comments):
Beneficiary’s name:
MTÜ VOLNA WITH UKRAINE TO VICTORY AND PROSPERITY
Reg. No: 80646495
IBAN: EE432200221088952836
Address: Parnu mnt. 82-96, Tallinn, Harjumaa, 10131, Estonia
Bank: SWEDBANK
SWIFT/BIC: HABAEE2X
Details: Donation for AO Trauma Ukraine
We currently need to raise €5,000 to restore the lower limb of a patient in a military hospital (RIA-2 plus BONALIVE in granules and paste). We sincerely hope for your support!
Now, here’s an example where additional support is not needed.
One of the foundations (enormous thanks!) has already covered the major expenses.
But it serves as a good example of upper limb salvage as a multi-stage process.
A soldier (now demobilized) sustained a blast injury in February of this year.
Six procedures were initially performed to begin the limb-salvage process for the arm (external fixation and wound debridement).
Despite the wound becoming infected with a “military” bacterium (American surgeons refer to this and Acinetobacter as the “Iraq bacteria” or “veterans’ disease”), Ukrainian doctors were able to manage the infection.
Simultaneously, several skin grafting procedures were carried out. One of Ukraine’s best plastic surgeons performed a thoracodorsal flap. The wounds have healed. The patient was transferred to us after 6 weeks of rehabilitation.
But the “Iraq bacterium” (named after the experience of wounded U.S. veterans) proved to be a particularly insidious microorganism.
So, together with Vasyl Parii and Denys Dolgush, instead of performing massive bone grafting immediately, we decided to stabilize the severely damaged humerus (see X-rays) with a plate using a minimally invasive approach — and took new tissue samples for culture. In peacetime and in case of a normal civilian injury (usually the main bacteria in such cases is Staphylococcus Aureus), we would do bone grafting simultaneously with internal fixation. But the presence of the “Iraqi bacteria” in early investigations does not allow this; the risk of severe complications is too high.
If the cultures come back sterile, we’ll proceed with the grafting.
If not, we’ll continue with aggressive antibiotic therapy.
Then, surgery on the brachial plexus will be necessary (there is a nerve injury).
If all goes well, we will work with the patient to determine what to do about the shoulder joint.
Most likely, it will need to be fused (arthrodesis surgical procedure) — the deltoid muscle and parts of the rotator cuff are missing, and we still don’t know the full extent of nerve recovery (although there’s some positive progress).
We’ll see.
Thank you all for your support!
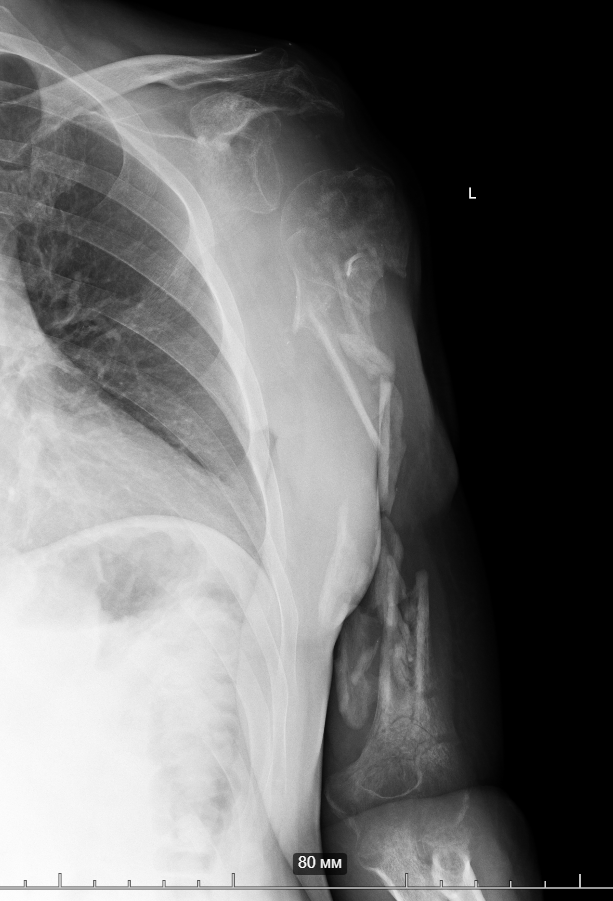
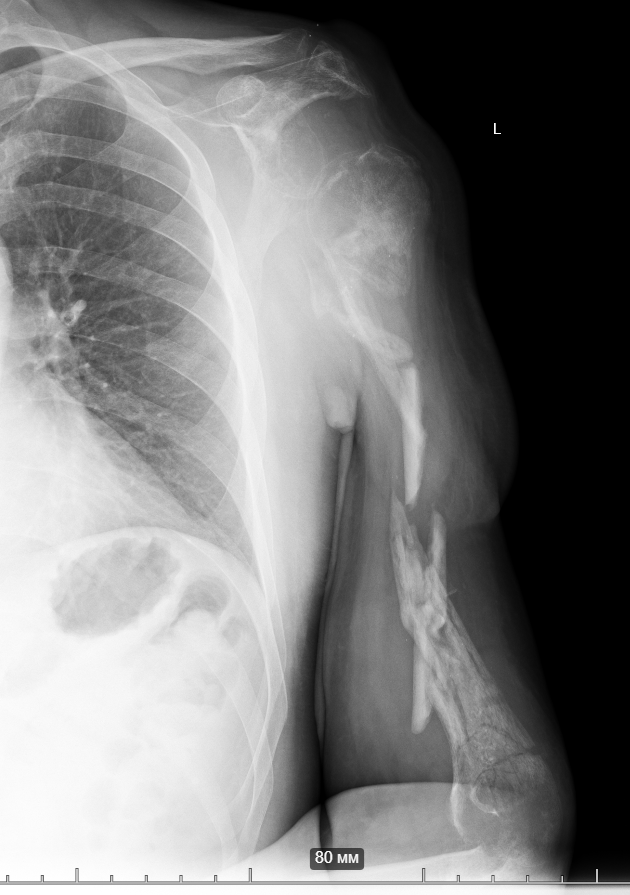
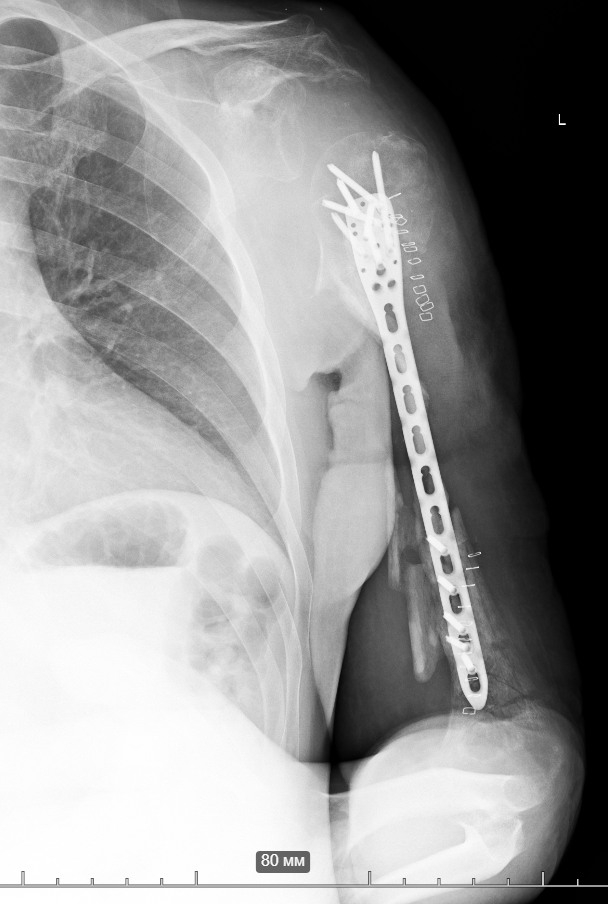
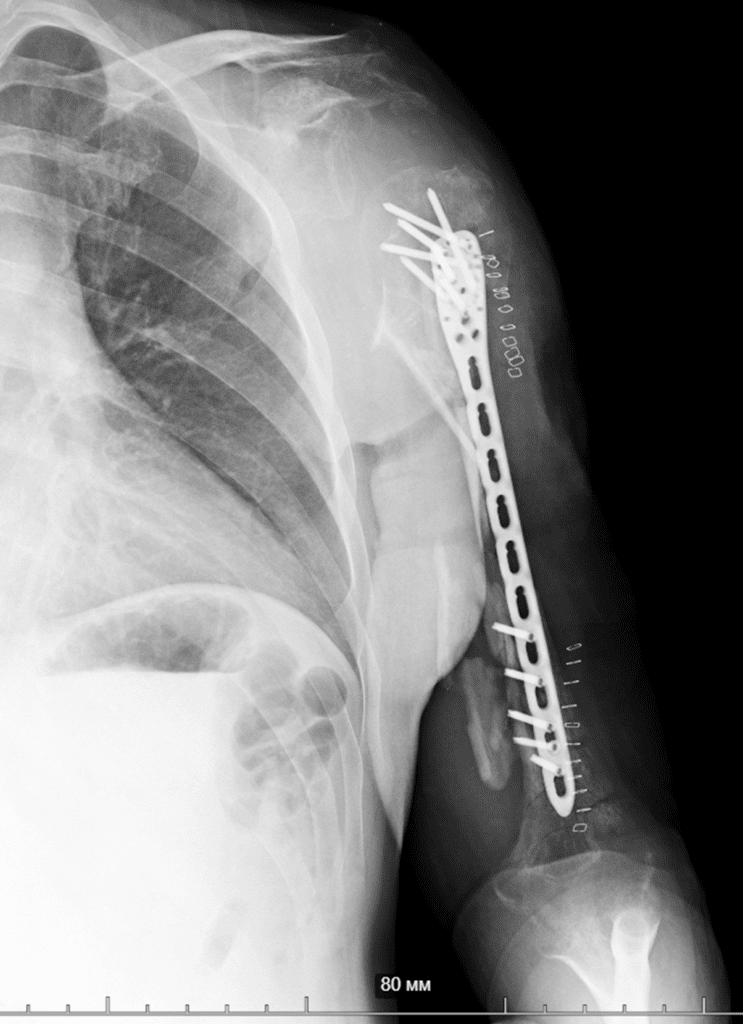
9.12.2024 Case N1
Author: Petro Nikitin. Автор: Петро Нiкiтiн.
Soldier, 27 years old
Injury 5 days before admission to the Central Military Hospital (before admission at the battlefield hospital: Debridement of the right lower leg, ExFix; amputation of the left lower leg).
Diagnosis: Blust shrapnel injury: Complex (multi-fragmentary) fracture of the distal epimetaphysis of tibia and fibula with primary defect of the soft tissues and bone; injury of posterior tibial and peroneal arteries, posterior tibial and peroneal nerves and Achilles tendon.
Photo 1, 2, 3, 4
Солдат, ДПСУ, 27 р.
Травма 5 діб до поступлення в ЦКГ ДПСУ (Ранiше: «ПХО», АЗФ правої гомілки; Ампутація лівої гомілки ).
Діагноз: Вогнепальне осколкове наскрізне поранення лівої гомілки, багатоуламковий перелом дистального епіметафізу обох кісток гомілки з дефектом м’яких тканин та кістки; пошкодження задньої великогомілкової та малогомілкової артерій, заднього великогомілкового та малогомілкового нервів і Ахіллового сухожилка. Травматичний дефект лівої гомілки
Photo 1, 2, 3, 4
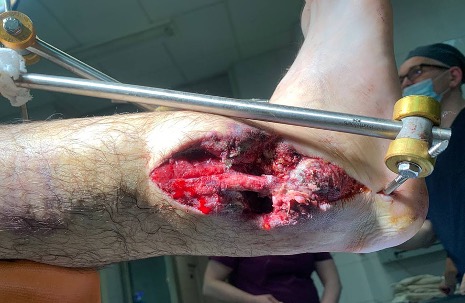


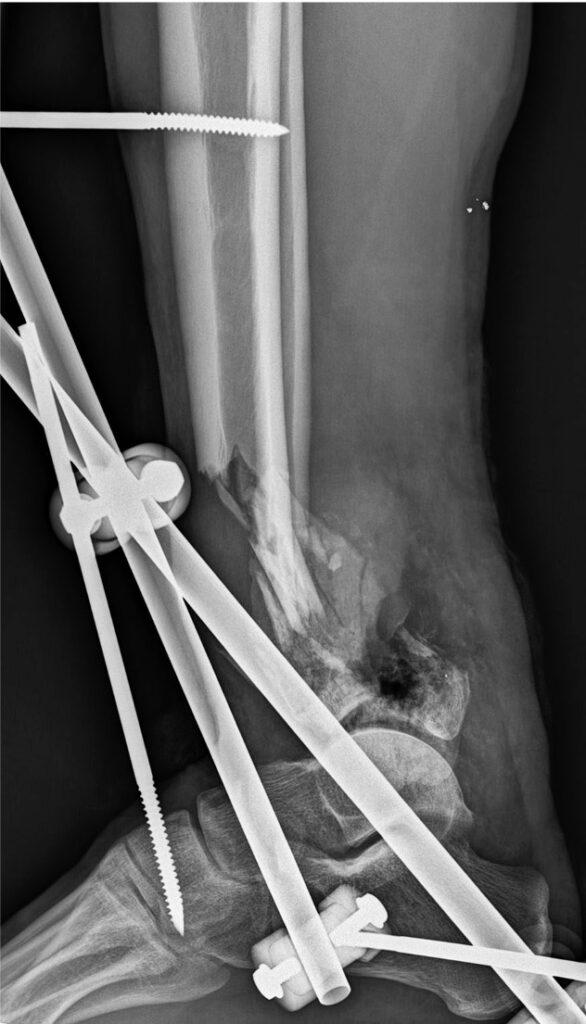
Upon admission: 2nd debridement, ExFix changing, VAC therapy
Photo 5, 6, 7
При поступленні: редебридемент, перемонтаж АЗФ, VAC
Photo 5, 6, 7
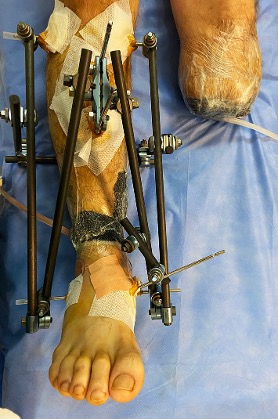
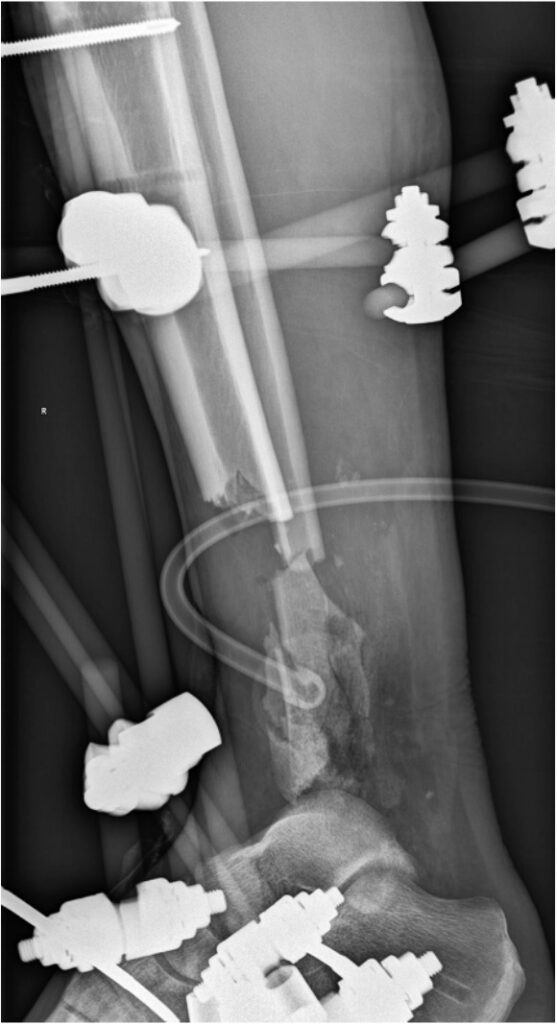
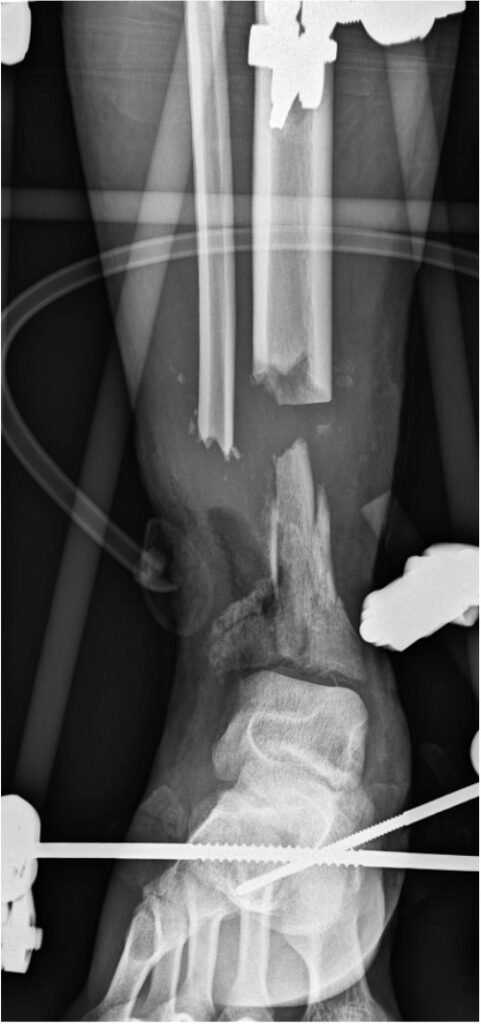
9 days after admission: 3rd debridement, solid cement spacer with antibiotic and TEN, VAC.
Photo 8, 9, 10
9 доба після поступлення: редебридмент, цільний цементний спейсер з антибіотиком і TEN, VAC.
Photo 8, 9, 10
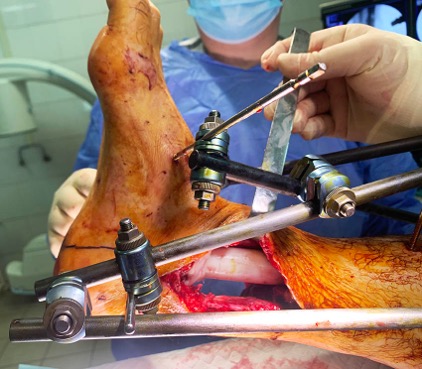

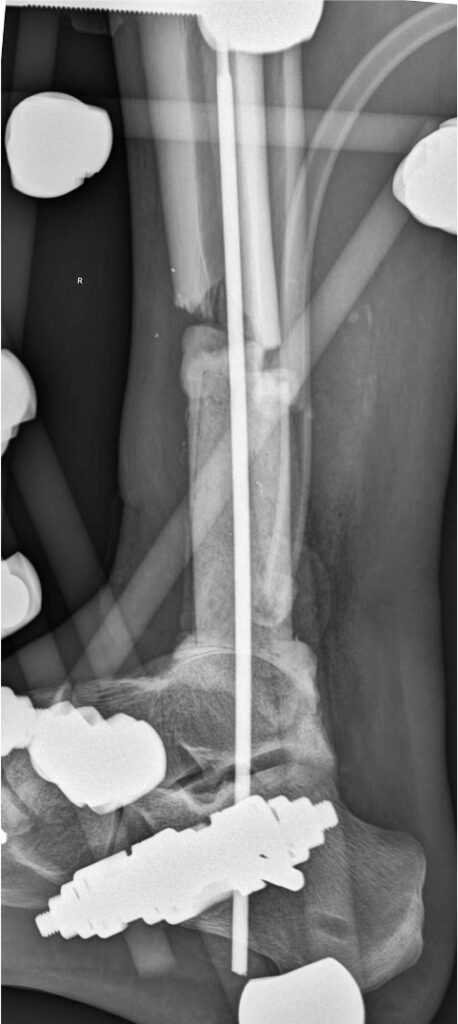
18 days after admission: 4th debridement, closure of the soft tissue defect with a full fasciocutaneous vascular sural flap
Photo 11
18 доба після поступлення: редебридмент, закриття дефекту м’яких тканин латеральної поверхні гомілки повношаровим суральним клаптем на судинній ніжці
Photo 11

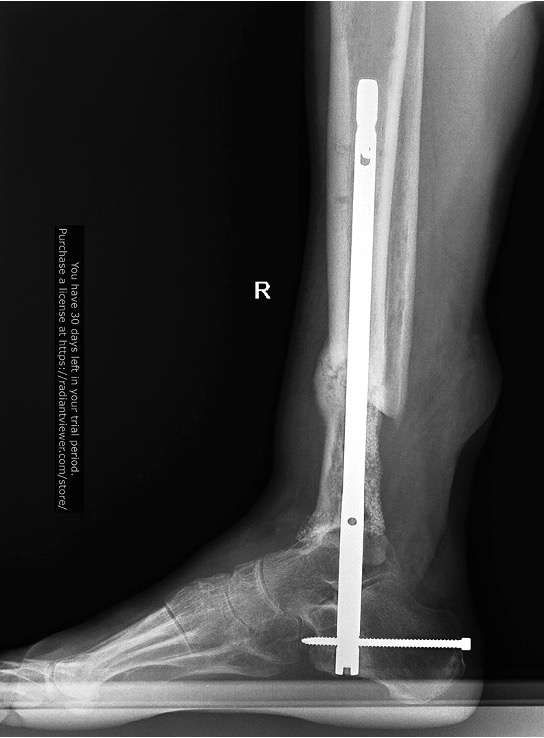
86 days after admission: Masquelet surgical technique: cement spacer removal, transarticular IMN, bone grafting using RIA 2 system plus “BonAlive” bioglass
Photo 12, 13
86 доба після поступлення: видалення цементного спейсера, трансартикулярна фіксація відп’ятковим інтрамедулярним блокованим стержнем; кісткова аутопластика RIA 2 + біоскло “BonAlive”
Photo 12, 13

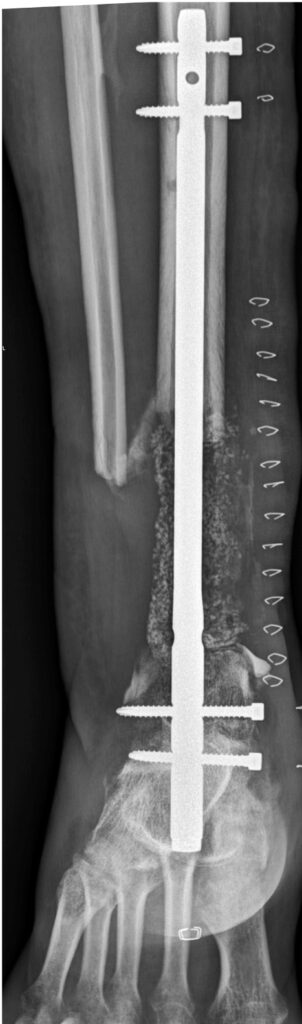
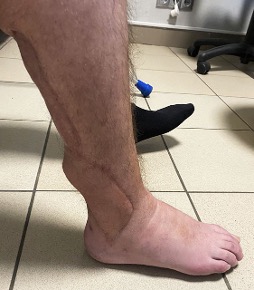
1 year after injury: Physically and socially rehabilitated. Started working at a defense enterprise. Got married.
Photo 14, 15, 16, 17, 18
1 рік після поранення: Фізично та соціально реабілітований. Почав працювати на оборонному підприємстві. Одружився.
Photo 14, 15, 16, 17, 18



Designed by Vera Volna
